Behavioral Health IntelliScan™
Enabling Payers to rapidly pinpoint provider outliers and uncover cost-savings in behavioral health claims

Behavioral health costs for payers are rising sharply; driven by increased utilization, regulatory complexity, and expanded access to care. Traditional payment integrity solutions often overlook behavioral health, leaving payers exposed to costly gaps in accuracy, compliance, and oversight.
Behavioral Health IntelliScan™ combines proprietary analytics with deep clinical and market expertise to close gaps, and detect and remediate costly errors while maintaining compliance and supporting sustainable care delivery.
Our Behavioral Health Approach
AArete’s proprietary Behavioral Health IntelliScan™, an AI-powered analytics tool, reduces costs while improving access and outcomes for members with behavioral conditions, lending value across the payer enterprise, including:
By doing so, AArete is uniquely positioned to help health plans with:
- Holistic Claims Oversight
- Reviews plan, provider, and member-level claims data to detect anomalies and misaligned reimbursement.
- Behavioral Health-Specific Analytics
- Proprietary edits and advanced detection identify overpayments, upcoding, inappropriate units, and policy misalignment.
- Policy & Benefit Alignment
- Evaluates service limits, prior authorization requirements, and network participation against CMS, state, and plan guidelines.

Behavioral Health Opportunity Areas For Payers

Provider Outliers
Detect providers whose billing patterns deviate significantly from peers, flagging potential fraud, waste, or abuse.

Procedure Level Anomalies
Highlights specific CPT/HCPCS codes with unusually high utilization or cost, often tied to behavioral health services.

Policy Misalignment
Surfaces claims that may not align with payer policies or clinical guidelines, enabling targeted policy updates.

Overpayment Recovery Options
Quantifies potential recoverable dollars by identifying inappropriate billing or coding practices.
Why AArete?
AArete has decades of experience working with payers to solve the complexities of behavioral health. Our Behavioral Health Payment IntelliScan™ solution is:

Configurable
To client-specific policies, contracts, and state requirements.

Proven
To reduce costs and inappropriate utilization while maintaining member outcomes.

Sustainable
Delivering savings in months and enabling long-term operational improvements.
Our Behavioral Health Experts
1. Centers for Disease Control and Prevention. Mental Health-Related Emergency Department Visits. Percentage generated by summing total related ED visits including mental health, anxiety, depression, trauma and stressor disorders, bipolar disorders, and schizophrenia spectrum disorders. Accessed October 2025. Available: cdc.gov
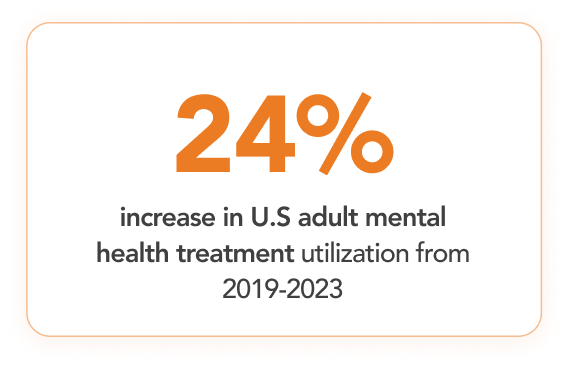
2. Centers for Disease Control and Prevention, National Center for Health Statistics (NCHS). QuickStats: Mental Health Treatment Among Adults — United States, 2019–2023. Accessed October 2025. Available: cdc.gov
3. Soni, A. Healthcare Expenditures for Treatment of Mental Disorders: Estimates for Adults 18+, U.S. (2019). Statistical Brief #539. Agency for Healthcare Research and Quality (AHRQ). Accessed October 2025. Available: meps.ahrq.gov